Breathing Overlap Profiles phenotype
Bison: Apnea-Insomnia Overlap
Your nights may combine airway strain with trouble falling asleep or settling back down.
These animals combine sleep-disordered breathing with position, insomnia, alcohol, jaw tension, self-wakening, or atypical respiratory patterns.


Interpretation
How to read this phenotype
Your nights may combine airway strain with trouble falling asleep or settling back down. [1] [2]
Read this phenotype as an overlap, not a single label. Airway problems often mix with position, insomnia, alcohol, jaw tension, or self-awakenings in ways that make the night look messier than one diagnosis alone. That overlap matters because the best next step depends on which part of the pattern is doing the most damage right now: breathing strain, position, repeated wake-ups, or something layered on top of the airway issue. A rough morning can come from repeated breathing strain and micro-disruption even when the sleeper does not remember many awakenings. [3] [4] [5]
Deep sleep is not just about logging enough hours; it is where the night often becomes truly restorative. That is where SleepSpace becomes more useful than a static score alone: it can help you see the pattern more clearly and, when appropriate, respond in real time with sound and light changes while the night is still unfolding. [6]
What this often looks like
Common signals in real life
- Your nights may combine airway strain with trouble falling asleep or settling back down.
- Airway strain often overlaps with another modifier such as position, insomnia, alcohol, or jaw tension.
- The overlap matters because it changes how the night feels and how the next step should be framed.
- The page should teach the sleeper what to monitor without pretending a single pattern explains everything.
- Screening, adherence, and anatomy-sensitive interpretation often matter more here than generic sleep hygiene.
Why this page exists
What makes Bison distinct
The pages should teach without sounding alarmist: enough specificity to prompt evaluation, but still readable.
Treat airway evaluation and insomnia support as parallel tracks. SleepSpace can help stabilize the behavioral side while you investigate breathing-related disruption.
Scientific read
Overlap breathing profiles matter because airway problems do not arrive in one neat format. The same sleeper can have breathing instability plus insomnia, position sensitivity, alcohol effects, or repeated self-awakenings. That is why the literature here spans more than one lane: anatomy, position, device response, treatment adherence, and cardiovascular consequences all help describe different parts of the same night. This also explains why one person may mainly notice snoring and another mostly notices fatigue, headaches, dry mouth, or a miserable morning even without dramatic awakenings. The practical lesson is that overlap pages need more than one clue before the next step is obvious. The payoff is that once the right overlap is named, the right intervention gets clearer fast. [7] [10] [13] [16]
These are the pages where partner observations and multi-night trends can be especially helpful. Overlap papers matter because many breathing-related sleepers do not arrive with one neat textbook problem. They arrive with airway clues layered on top of another bottleneck. The payoff is that once the right overlap gets named, the next step stops feeling generic and starts feeling specific. A rough morning can come from repeated breathing strain and micro-disruption even when the sleeper does not remember many awakenings. [8] [11] [14] [17]
Deep sleep is not just about logging enough hours; it is where the night often becomes truly restorative. Strategic naps can restore more than people expect when the alternative is trying to grind through a biologically low period. A recurring finding in the sleep-loss literature is that people feel more adapted than their attention, mood, and reaction time really are. Overlap breathing profiles matter because airway problems do not arrive in one neat format. The same sleeper can have breathing instability plus insomnia, position sensitivity, alcohol effects, or repeated self-awakenings. [9] [12] [15] [18]
Tracking and wearables
What data often helps separate this pattern from nearby ones
Because these patterns change with context, the best data are often multi-night and multi-setting: travel versus home, stressful versus calm weeks, winter versus summer, and high-demand versus lower-demand periods. [14]
SleepSpace's own tracking and wearables articles are especially relevant for these pages because they reinforce the difference between a one-night impression and an interpretable pattern. That is useful for every phenotype, but it becomes essential when the mechanism changes with context. [12] [14] [13]

SleepSpace app features
Use these tools if you want to improve this pattern instead of just reading about it
Start with the assessment, download the app, and use the features below to turn this sleep animal into a practical plan.

SleepSpace feature
Sleep assessment
Start here if you want a clearer read on your sleep animal, your main bottlenecks, and what to work on first.
Learn how to use it
SleepSpace feature
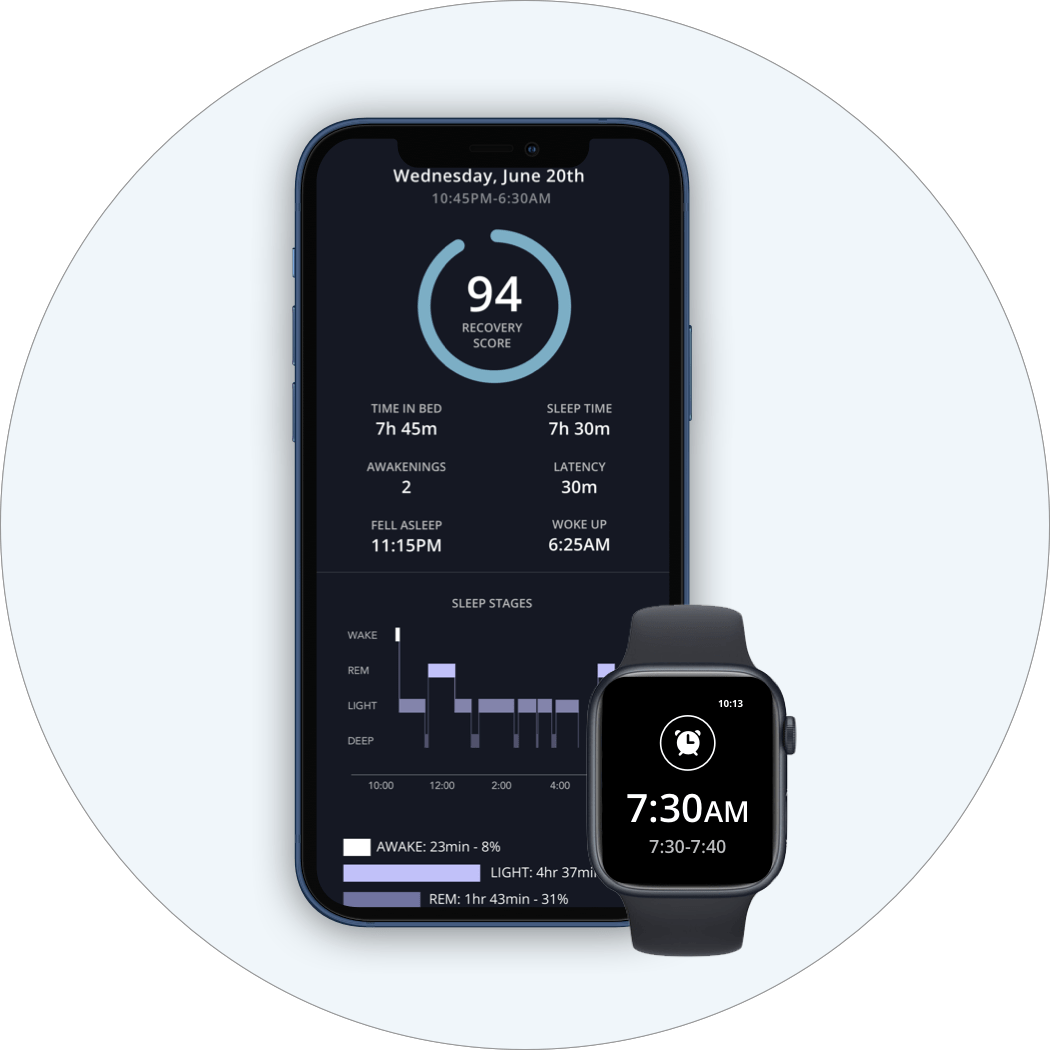
Sleep diary
Use the diary to catch patterns in timing, awakenings, stress, recovery, and what actually changed from one night to the next.
Learn how to use it
SleepSpace feature
24/7 sleep support
Use guided support when you need help calming the mind, sticking with the plan, or getting out of a rough stretch faster.
Learn how to use it
SleepSpace resources
SleepSpace resources that fit this phenotype
These were selected by spidering SleepSpace topic pages and product resources that match the mechanism cluster behind this animal.
SleepSpace article
SleepSpace learning hub
A broad SleepSpace article library that can serve as the hub resource on every page.
SleepSpace article
SleepSpace science page
Useful when the page needs a product-adjacent evidence destination.
SleepSpace article
Snoring and breathing tracking guide
Useful for airway, snoring, and breathing-disruption pages.
SleepSpace article
Tracking and wearables guide
Useful for pages that emphasize data quality, sleep diaries, and wearables.
FAQ
Questions Dr. Dan would expect about this animal
Quick answers to the questions people usually ask when this sleep pattern feels familiar.
What does the Bison sleep animal mean?
This overlap profile reflects both breathing-related signals and insomnia-like arousal. People here can feel caught in the middle: tired enough to need help, but too activated or disrupted to sleep smoothly. The right plan usually needs to respect both sides instead of treating the issue as only one or the other. This phenotype is especially important because one problem can easily hide behind the other if you are not looking for both. This long-form page treats Bison as a sleep phenotype: a memorable wrapper around a recurring pattern that likely clusters across schedule, physiology, stress load, and next-day restoration. The goal is not to claim a formal diagnosis. The goal is to make the likely mechanism more understandable and the next step more obvious. This is educational guidance to help you recognize the pattern, not a medical diagnosis.
What should you track if this bison pattern sounds like you?
Because these patterns change with context, the best data are often multi-night and multi-setting: travel versus home, stressful versus calm weeks, winter versus summer, and high-demand versus lower-demand periods. [14] Start with the SleepSpace sleep assessment and then use the app to watch what happens to timing, continuity, symptoms, and next-day recovery over time.
When should you get extra help for bison-style sleep problems?
If this pattern is getting more intense, affecting safety, or leaving you persistently exhausted, treat this page as educational and talk with a doctor or sleep specialist. SleepSpace can help you organize the pattern, but medical concerns still deserve medical care.
Important note
Address both sides of the night
If loud snoring, observed breathing pauses, gasping, severe daytime sleepiness, or blood-pressure concerns are part of the story, a formal sleep evaluation matters. These pages can orient the sleeper, but they do not replace diagnostic workup for sleep-disordered breathing. [11] [10]
Use SleepSpace to support more stable sleep while pursuing the right airway follow-up.
Research references
Selected citations for this page
Show citations (18)
- Nsair et al. (2019). Factors Influencing Adherence to Auto-CPAP: An Observational Monocentric Study Comparing Patients With and Without Cardiovascular Diseases.
A rough morning can come from repeated breathing strain and micro-disruption even when the sleeper does not remember many awakenings.
Full article - Rapelli et al. (2021). Improving CPAP Adherence in Adults With Obstructive Sleep Apnea Syndrome: A Scoping Review of Motivational Interventions.
This trial is especially relevant because a rough morning can come from repeated breathing strain and micro-disruption even when the sleeper does not remember many awakenings.
Full article - Chong et al. (2006). Continuous positive airway pressure reduces subjective daytime sleepiness in patients with mild to moderate Alzheimer's disease with sleep disordered breathing.
This trial is especially relevant because deep sleep is not just about logging enough hours; it is where the night often becomes truly restorative.
Full article - Labarca et al. (2022). Mouth Closing to Improve the Efficacy of Mandibular Advancement Devices in Sleep Apnea.
Deep sleep is not just about logging enough hours; it is where the night often becomes truly restorative.
Full article - Rosenberg et al. (2007). A pilot study evaluating acute use of eszopiclone in patients with mild to moderate obstructive sleep apnea syndrome.
This trial is especially relevant because a rough morning can come from repeated breathing strain and micro-disruption even when the sleeper does not remember many awakenings.
Full article - Sivertsen et al. (2013). The joint contribution of insomnia and obstructive sleep apnoea on sickness absence.
The night can become self-reinforcing when the bed turns into a place for monitoring, rehearsing, and trying too hard.
Full article - Series et al. (2005). Prospective evaluation of nocturnal oximetry for detection of sleep-related breathing disturbances in patients with chronic heart failure.
This trial is especially relevant because a rough morning can come from repeated breathing strain and micro-disruption even when the sleeper does not remember many awakenings.
Full article - Huang et al. (2005). The impact of anatomic manipulations on pharyngeal collapse: results from a computational model of the normal human upper airway.
A rough morning can come from repeated breathing strain and micro-disruption even when the sleeper does not remember many awakenings.
Full article - Kezirian et al. (2010). Changes in obstructive sleep apnea severity, biomarkers, and quality of life after multilevel surgery.
A rough morning can come from repeated breathing strain and micro-disruption even when the sleeper does not remember many awakenings.
Full article - Seixas et al. (2018). Culturally tailored, peer-based sleep health education and social support to increase obstructive sleep apnea assessment and treatment adherence among a community sample of blacks: study protocol for a randomized controlled trial.
This trial is especially relevant because deep sleep is not just about logging enough hours; it is where the night often becomes truly restorative.
Full article - Turino et al. (2017). Management of continuous positive airway pressure treatment compliance using telemonitoring in obstructive sleep apnoea.
Strategic naps can restore more than people expect when the alternative is trying to grind through a biologically low period.
Full article - Swanson et al. (2011). Sleep disorders and work performance: findings from the 2008 National Sleep Foundation Sleep in America poll.
A recurring finding in the sleep-loss literature is that people feel more adapted than their attention, mood, and reaction time really are.
Full article - Newman et al. (2000). Daytime sleepiness predicts mortality and cardiovascular disease in older adults. The Cardiovascular Health Study Research Group.
A rough morning can come from repeated breathing strain and micro-disruption even when the sleeper does not remember many awakenings.
Full article - Kaditis et al. (2010). Associations of tonsillar hypertrophy and snoring with history of wheezing in childhood.
A rough morning can come from repeated breathing strain and micro-disruption even when the sleeper does not remember many awakenings.
Full article - Gozal et al. (2013). Chemoreceptors, baroreceptors, and autonomic deregulation in children with obstructive sleep apnea.
A rough morning can come from repeated breathing strain and micro-disruption even when the sleeper does not remember many awakenings.
Full article - Yumino et al. (2013). Differing effects of obstructive and central sleep apneas on stroke volume in patients with heart failure.
A rough morning can come from repeated breathing strain and micro-disruption even when the sleeper does not remember many awakenings.
Full article - Berlowitz et al. (2012). Relationships between objective sleep indices and symptoms in a community sample of people with tetraplegia.
A rough morning can come from repeated breathing strain and micro-disruption even when the sleeper does not remember many awakenings.
Full article - Jordan et al. (2007). Mechanisms used to restore ventilation after partial upper airway collapse during sleep in humans.
A rough morning can come from repeated breathing strain and micro-disruption even when the sleeper does not remember many awakenings.
Full article
Nearby profiles


