Airway, Environment, and Physical Load phenotype
Porcupine: Pain Tosser
Your body may be interrupting your sleep before your brain gets the chance to settle.
The recurring theme here is that the body or the room keeps breaking the night apart: breathing strain, pain, heat, noise, movement, or bed-partner disruption.

Interpretation
How to read this phenotype
Your body may be interrupting your sleep before your brain gets the chance to settle. [1] [2]
Read this phenotype by asking what keeps breaking continuity. If breathing effort, sound, pain, movement, or temperature keeps pulling the body upward, the morning can feel much worse than the clock suggests. This group usually improves once the main disruptor gets named clearly. Generic sleep tips matter less when the real bottleneck is physical, positional, or environmental. Deep sleep is not just about logging enough hours; it is where the night often becomes truly restorative. [3] [4] [5]
The sleeper may not remember dramatic awakenings, yet the body can still be leaving deep recovery over and over again. A rough morning can come from repeated breathing strain and micro-disruption even when the sleeper does not remember many awakenings. That is where SleepSpace becomes more useful than a static score alone: it can help you see the pattern more clearly and, when appropriate, respond in real time with sound and light changes while the night is still unfolding. [6]
What this often looks like
Common signals in real life
- Your body may be interrupting your sleep before your brain gets the chance to settle.
- The body or the room keeps disturbing the night, even if total time in bed looks adequate.
- The sleeper may not always recognize the night as fragmented until daytime restoration drops.
- Not every page in this cluster implies the same level of medical urgency, but many benefit from screening.
- Environment, position, pain load, sound, and partner factors can all amplify the core problem.
Why this page exists
What makes Porcupine distinct
This cluster needs practical realism: some causes are behavioral, some need screening, and many overlap.
Focus on making sleep easier on your body and less reactive for your brain. SleepSpace can support pre-sleep relaxation, environmental optimization, and a more restorative nightly pattern.
Scientific read
These profiles are often about fragmentation happening below awareness. The sleeper may not remember many long awakenings, yet the night still keeps stepping out of deeper recovery. Breathing papers matter because airway strain can hide behind snoring, dry mouth, morning heaviness, headaches, or a partner’s observations rather than dramatic self-reported wake-ups. Environmental and physical-disruption papers matter because temperature, pain, movement, and noise can create the same under-restored morning without looking identical on the surface. This is why the right question is not just whether you slept. It is what kept nudging the body out of stable recovery over and over again. [7] [10] [13] [16]
A practical theme in this literature is that position, sound, and physical setup can change the night more than people expect. These papers are useful because they explain how a night can be disrupted below awareness. The sleeper may not recall long awakenings, yet the body keeps getting tugged out of deeper recovery. That is why sound, position, pain, heat, breathing effort, and partner observations all matter here instead of just the total hours in bed. A rough morning can come from repeated breathing strain and micro-disruption even when the sleeper does not remember many awakenings. [8] [11] [14] [17]
The sleeper may not remember dramatic awakenings, yet the body can still be leaving deep recovery over and over again. Deep sleep is not just about logging enough hours; it is where the night often becomes truly restorative. Small thermal disruptions can keep sleep lighter than the clock would suggest, especially in the second half of the night. The room itself can become the bottleneck when sound or unpredictability keeps the nervous system slightly on guard. [9] [12] [15] [18]
Tracking and wearables
What data often helps separate this pattern from nearby ones
For these pages, useful data include sound events, snoring patterns, room conditions, awakenings, position notes, partner disturbance, and how often the sleeper wakes unrefreshed despite apparently adequate time in bed. [5] [11]
SleepSpace's own tracking and wearables articles are especially relevant for these pages because they reinforce the difference between a one-night impression and an interpretable pattern. That is useful for every phenotype, but it becomes essential when the mechanism changes with context. [9] [11] [10]

SleepSpace app features
Use these tools if you want to improve this pattern instead of just reading about it
Start with the assessment, download the app, and use the features below to turn this sleep animal into a practical plan.
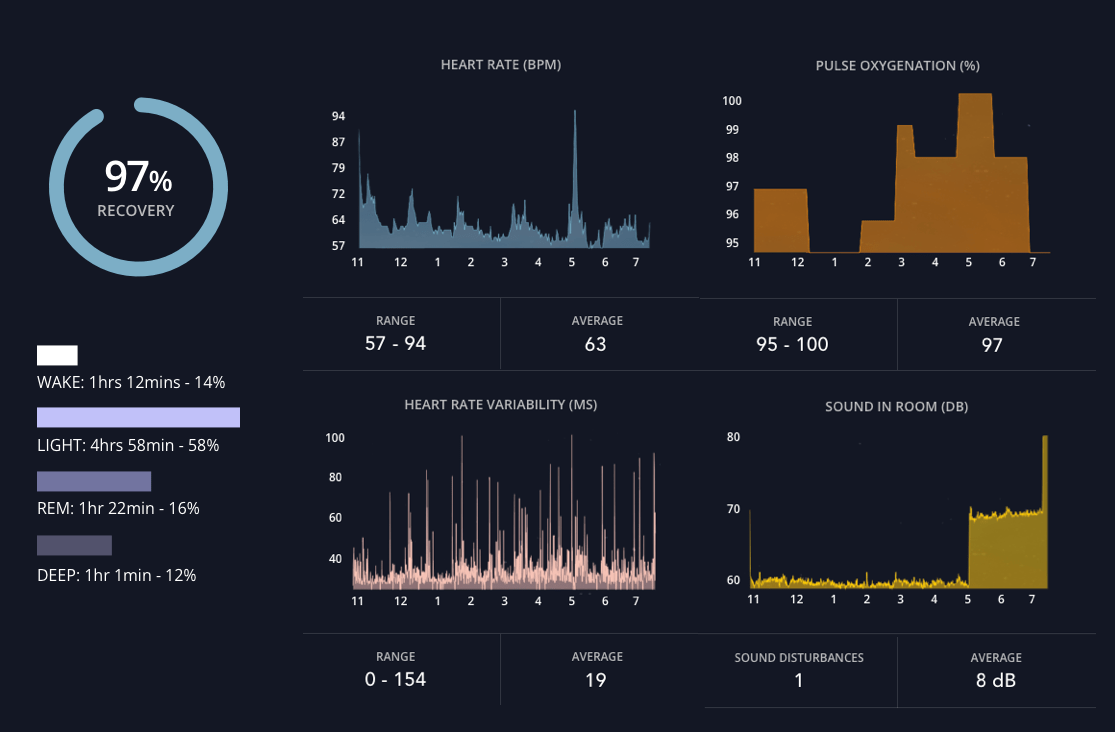
SleepSpace feature
Sleep assessment
Start here if you want a clearer read on your sleep animal, your main bottlenecks, and what to work on first.
Learn how to use it

SleepSpace feature
Sleep diary
Use the diary to catch patterns in timing, awakenings, stress, recovery, and what actually changed from one night to the next.
Learn how to use it

SleepSpace feature
Weekly sleep stats
Use weekly trends to see whether you are actually improving instead of judging everything from one rough night.
Learn how to use it
SleepSpace resources
SleepSpace resources that fit this phenotype
These were selected by spidering SleepSpace topic pages and product resources that match the mechanism cluster behind this animal.
SleepSpace article
SleepSpace learning hub
A broad SleepSpace article library that can serve as the hub resource on every page.
SleepSpace article
SleepSpace science page
Useful when the page needs a product-adjacent evidence destination.
SleepSpace article
Snoring and breathing tracking guide
Useful for airway, snoring, and breathing-disruption pages.
SleepSpace article
Sound masking guide
Useful for noise, partner, and light-sleeper pages.
SleepSpace article
Tracking and wearables guide
Useful for pages that emphasize data quality, sleep diaries, and wearables.
FAQ
Questions Dr. Dan would expect about this animal
Quick answers to the questions people usually ask when this sleep pattern feels familiar.
What does the Porcupine sleep animal mean?
Pain-driven sleep disruption often looks like frequent position changes, light sleep, short awakenings, or difficulty staying comfortable long enough to rest deeply. That can become frustrating because it makes bedtime feel effortful and recovery incomplete. When pain and sleep feed each other, nights often need a more supportive strategy. The right solution usually combines comfort, routine, and a more calming sleep environment. Better sleep here often begins with reducing the amount of negotiation your body has to do all night long. This long-form page treats Porcupine as a sleep phenotype: a memorable wrapper around a recurring pattern that likely clusters across schedule, physiology, stress load, and next-day restoration. The goal is not to claim a formal diagnosis. The goal is to make the likely mechanism more understandable and the next step more obvious. This is educational guidance to help you recognize the pattern, not a medical diagnosis.
What should you track if this porcupine pattern sounds like you?
For these pages, useful data include sound events, snoring patterns, room conditions, awakenings, position notes, partner disturbance, and how often the sleeper wakes unrefreshed despite apparently adequate time in bed. [5] [11] Start with the SleepSpace sleep assessment and then use the app to watch what happens to timing, continuity, symptoms, and next-day recovery over time.
When should you get extra help for porcupine-style sleep problems?
If this pattern is getting more intense, affecting safety, or leaving you persistently exhausted, treat this page as educational and talk with a doctor or sleep specialist. SleepSpace can help you organize the pattern, but medical concerns still deserve medical care.
Important note
Help your body stop interrupting the night
If loud snoring, observed breathing pauses, gasping, severe daytime sleepiness, or blood-pressure concerns are part of the story, a formal sleep evaluation matters. These pages can orient the sleeper, but they do not replace diagnostic workup for sleep-disordered breathing. [7]
Use SleepSpace to create a calmer, more restorative routine when pain is getting in the way of sleep.
Research references
Selected citations for this page
Show citations (18)
- Bartels et al. (2016). Definition and Importance of Autonomic Arousal in Patients with Sleep Disordered Breathing.
Deep sleep is not just about logging enough hours; it is where the night often becomes truly restorative.
Full article - Kim et al. (2012). Association between work-family conflict and musculoskeletal pain among hospital patient care workers.
The sleeper may not remember dramatic awakenings, yet the body can still be leaving deep recovery over and over again.
Full article - Rosenberg et al. (2007). A pilot study evaluating acute use of eszopiclone in patients with mild to moderate obstructive sleep apnea syndrome.
This trial is especially relevant because a rough morning can come from repeated breathing strain and micro-disruption even when the sleeper does not remember many awakenings.
Full article - Olson et al. (2006). Modulation of cardiovascular risk factors by obstructive sleep apnea.
A rough morning can come from repeated breathing strain and micro-disruption even when the sleeper does not remember many awakenings.
Full article - Caples et al. (2005). Obstructive sleep apnea.
Strategic naps can restore more than people expect when the alternative is trying to grind through a biologically low period.
Full article - Torelli et al. (2011). Cognitive profile and brain morphological changes in obstructive sleep apnea.
A rough morning can come from repeated breathing strain and micro-disruption even when the sleeper does not remember many awakenings.
Full article - Quan et al. (2012). Obstructive Sleep Apnea and Cardiovascular Disease: Back and Forward in Time Over the Last 25 Years.
A rough morning can come from repeated breathing strain and micro-disruption even when the sleeper does not remember many awakenings.
Full article - Caldwell et al. (2009). Body mass index and quality of life: examining blacks and whites with chronic pain.
The sleeper may not remember dramatic awakenings, yet the body can still be leaving deep recovery over and over again.
Full article - Kezirian et al. (2010). Changes in obstructive sleep apnea severity, biomarkers, and quality of life after multilevel surgery.
A rough morning can come from repeated breathing strain and micro-disruption even when the sleeper does not remember many awakenings.
Full article - Seixas et al. (2018). Culturally tailored, peer-based sleep health education and social support to increase obstructive sleep apnea assessment and treatment adherence among a community sample of blacks: study protocol for a randomized controlled trial.
This trial is especially relevant because deep sleep is not just about logging enough hours; it is where the night often becomes truly restorative.
Full article - Hignett et al. (1996). Work-related back pain in nurses.
This review is useful because the sleeper may not remember dramatic awakenings, yet the body can still be leaving deep recovery over and over again.
Full article - Chou et al. (2002). Afferents to the ventrolateral preoptic nucleus.
Small thermal disruptions can keep sleep lighter than the clock would suggest, especially in the second half of the night.
Full article - Day et al. (1941). Regulation of body temperature during sleep.
Small thermal disruptions can keep sleep lighter than the clock would suggest, especially in the second half of the night.
Full article - Chen et al. (2021). Does continuous positive airway pressure therapy benefit patients with coronary artery disease and obstructive sleep apnea? A systematic review and meta‐analysis.
This review is useful because deep sleep is not just about logging enough hours; it is where the night often becomes truly restorative.
Full article - Roca et al. (2013). Sleep Apnea Is Associated with Subclinical Myocardial Injury in the Community. The ARIC-SHHS Study.
A rough morning can come from repeated breathing strain and micro-disruption even when the sleeper does not remember many awakenings.
Full article - Pentland et al. (1999). The impact of spinal cord injury on men's time use.
The room itself can become the bottleneck when sound or unpredictability keeps the nervous system slightly on guard.
Full article - Dawson et al. (2007). Interventions to prevent back pain and back injury in nurses: a systematic review.
This trial is especially relevant because the sleeper may not remember dramatic awakenings, yet the body can still be leaving deep recovery over and over again.
Full article - Wetter et al. (1999). A randomized controlled study of pergolide in patients with restless legs syndrome.
This trial is especially relevant because the body can keep pulling sleep back toward the surface through urges to move long before the mind realizes how broken the night has become.
Full article
Nearby profiles


